Nasal Surgeries & Procedures
Nasal obstruction can be caused by a deviated septum, turbinate swelling, nasal polyps, nasal tumors and malignancies as well as collapse of the nasal valve region. Here at Indigo ENT, we have several specialists can help quickly diagnose, treat and manage your symptoms to help you breath better. Below are several procedures we specialize in.
Rhinoplasty refers to plastic surgery on the external and/or internal structures of the nose. While this surgery can be performed for purely cosmetic reasons, it can also be performed to improve the breathing function and the appearance of the nose, termed Functional Rhinoplasty. It is typically performed through a series of internal (hidden) incisions, called a closed rhinoplasty approach. Occasionally, an additional small incision under the tip of the nose is required to allow for improved surgical access, called an open rhinoplasty approach. The closed approach rhinoplasty tends to allow for faster post-operative recovery times, reduced tip numbness and avoids visible scars. The correct choice of procedure depends on the nature of your nasal issues and will be discussed during your pre-operative consultation.
The nasal valve refers to two regions of the nose, the external and internal nasal valve. The external nasal valve is an area formed by the lateral crus of the alar (i.e., lower lateral) cartilage and its associated external and vestibular soft tissue coverings. It is loosely referred to as the nostril opening. The internal nasal valve is deeper in the nasal passage and is defined as the area formed by articulation of the anterior ridge of the upper lateral cartilage with the anterior septal edge. The internal nasal valve is typically the most narrow area of our nasal passage, and is prone to collapse or structural narrowing. Collapse can be caused by congenital and developmental factors, trauma, or surgery. The collapse can be fixed and permanent or dynamic with inspiration. Nasal valve surgery consists of a variety of different surgical techniques and is commonly performed in conjunction with functional rhinoplasty or septoplasty.
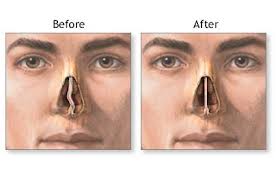
The nasal septum separates one side of the nose from the other with bone, cartilage, and overlying soft tissues. Blockage in the nose occurs with issues like septal deviation or septal spurs. A septoplasty attempts to straighten the septum and restore its position and open up the nasal airways.
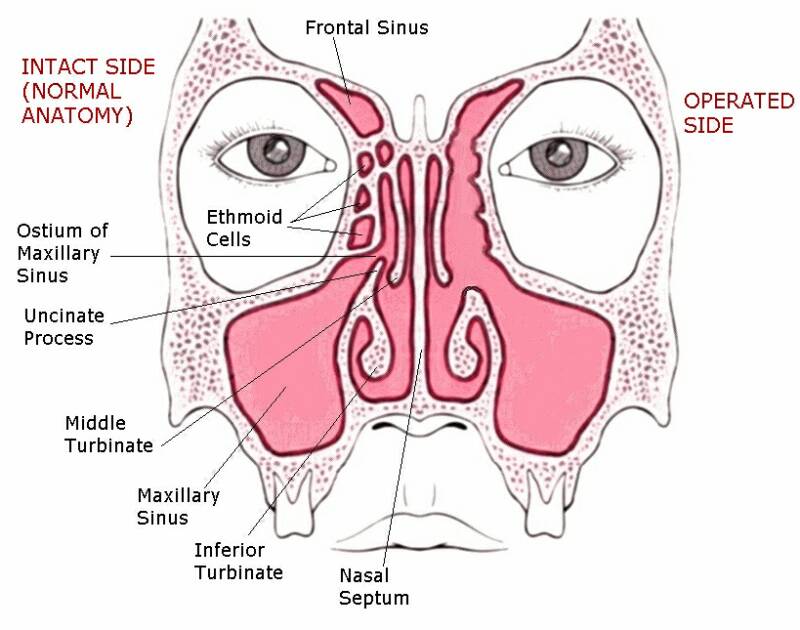 Using small telescopes to look into the nose, sinus surgery concerns removing small pieces of bone and lining (including any abnormalities) in order to widen the passageways that connect the sinuses to the nose. This surgery helps reduce the severity and frequency of sinus infections and improve the natural drainage of the sinuses. State of the art computer mapping software is routinely used during surgery to improve patient safety and the thoroughness of the surgery. Quality of life improvements after sinus surgery are well documented in the literature with improvements ranging from 50-97%. Significant improvement in pre-existing asthma and sleep quality is also well documented after endoscopic sinus surgery.
Using small telescopes to look into the nose, sinus surgery concerns removing small pieces of bone and lining (including any abnormalities) in order to widen the passageways that connect the sinuses to the nose. This surgery helps reduce the severity and frequency of sinus infections and improve the natural drainage of the sinuses. State of the art computer mapping software is routinely used during surgery to improve patient safety and the thoroughness of the surgery. Quality of life improvements after sinus surgery are well documented in the literature with improvements ranging from 50-97%. Significant improvement in pre-existing asthma and sleep quality is also well documented after endoscopic sinus surgery.
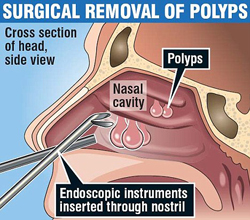 Nasal polyps are watery outgrowths from the lining of an inflamed nose. It typically correlates with chronic sinusitis and allergies. They can obstruct breathing and be a large source of discomfort and poor quality of life. If polyps are isolated, they can be easily grasped and removed with little to no discomfort.
Nasal polyps are watery outgrowths from the lining of an inflamed nose. It typically correlates with chronic sinusitis and allergies. They can obstruct breathing and be a large source of discomfort and poor quality of life. If polyps are isolated, they can be easily grasped and removed with little to no discomfort.
If polyps are numerous, sometimes obstructing the entire nasal cavity, we do offer the use of the Celeris Polyp Debrider. This is a unique microdebrider specifically tailored to remove polyps quickly and efficiently, under topical or local anesthetic. This provides an immediate significant improvement in breathing. The Celeris Polyp Debrider currently is not a benefit of MSP or covered through Third-party insurance. The cost of the unit is $700 and is one time use only.
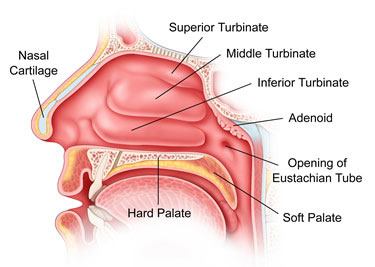
In the nasal cavity of the nose, there are three pairs of turbinates on the lateral walls. The inferior turbinates can be enlarged due to allergies, medications, or infection or irritants and can cause nasal obstruction. By reducing the size of turbinates, nasal blockage is demised and creates space for breathing.
Common turbinate surgeries include:
Submucous Resection
Performed in the operating room under general anesthesia, submucous resection involves making a cut in the lining of the inferior turbinates and lifting the lining off the thin bone, and inserting a specialized instrument called a microdebrider to remove the central tissue of the turbinate. This helps the nasal passage increase in size. This is often performed in combination with rhinoplasty, nasal septum or sinus surgery.
Coblation Turbinate Reduction
Usually performed in office under local anesthetic, coblation submucosal resection of the inferior turbinates and/or nasal septum provides excellent reduction in tissue volume. This typically increases nasal breathing significantly. Patients can resume typical activities (apart from heavy lifting) up to 15 minutes after the procedure. Evidence indicates quicker healing times than more traditional therapies. The procedure is a benefit of MSP however the specialized unit is a one time use only and currently is not covered by MSP or Third Party insurance. Cost for this unit is $400. Research shows long lasting benefit from this surgery after 32 months. It is possible that a repeat procedure will be required after several years.
View Turbinate Reduction Patient Brochure | View Turbinate Reduction Video
Radiofrequency Reduction
Usually performed in office with local anesthetic, radiofrequency reduction is where a probe with a needle is placed into the turbinate and radiofrequency energy is delivered to heat the tissues, acting as a catalyst to healing. This reduces the inferior turbinates. Patients can resume typical activities, while limiting heavy lifting, up to 15 minutes after the procedure. This procedure is covered by MSP. Like coblation turbinate reduction, the benefits are expected for at least several years. A repeat procedure may be required.
